Humble sleep
Ashish Bhatia, GP and founder of Humble
Published in JHH 18.2-Frontiers of self-care
Did you sleep well?
It’s such a simple question, rather like asking ‘how’s the weather’ or ‘how was your journey?’ Yet sleep is such a vital aspect of our lives that everyone seems to have a sleep story. Sleep is interconnected with all aspects of our health but increasingly it’s disturbed by our modern-day living (www.nhs.uk/live-well/sleep-and-tiredness/why-lack-of-sleep-is-bad-for-your-health).
This article aims to explore some of the science behind sleeping and not sleeping, the art of sleeping well, and to offer some practical tips to help you and those you care for sleep well.
There are lots of books on sleep (I found more than 60,000 on a google search!) each bursting with ideas. Notable among them is Why we Sleep by Matthew Walker (2018), which has had a tremendous impact in raising the profile of sleep. Unfortunately, I hear from my medical students, NHS and private sleep clients, that after reading this book they often lie in bed worrying about sleep, having learned of all the scary consequences of sleeping poorly. So let me first off give you the good news; sleep is a superpower which most people can improve.
The science of sleep made simple
I want to share some useful ideas and tips regarding sleep which I realise may look over-simplified and soon become outdated. Therefore, I very much welcome your feedback on this article so I can keep improving what I do.
What is sleep?
The Oxford dictionary defines it as, ‘a condition of body and mind that typically recurs for several hours every night, in which the nervous system is relatively inactive, the eyes closed, the postural muscles relaxed, and consciousness practically suspended’.
I find some of this definition incorrect or unhelpful.
1. ‘Typically several hours’ – although current health guidance is that adults should sleep at least seven hours and children for longer, most people are sleeping less and don’t realise it. The UK average is almost two hours less than recommended and two less than our grandparents. Indeed short sleeping has been called a public health crisis (Huberman, 2021; Chattu et al, 2018).
Sleep is not just on or off: its quality, timing and how we perceive it are important too. For example, the use of sedatives (like sleeping tablets and alcohol) interferes with the quality of our sleep. So though we may be unconscious, the full benefits of quality sleep maybe missing (Pagel & Parnes, 2001).
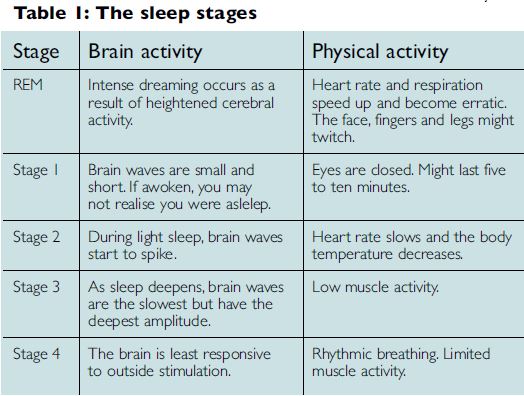
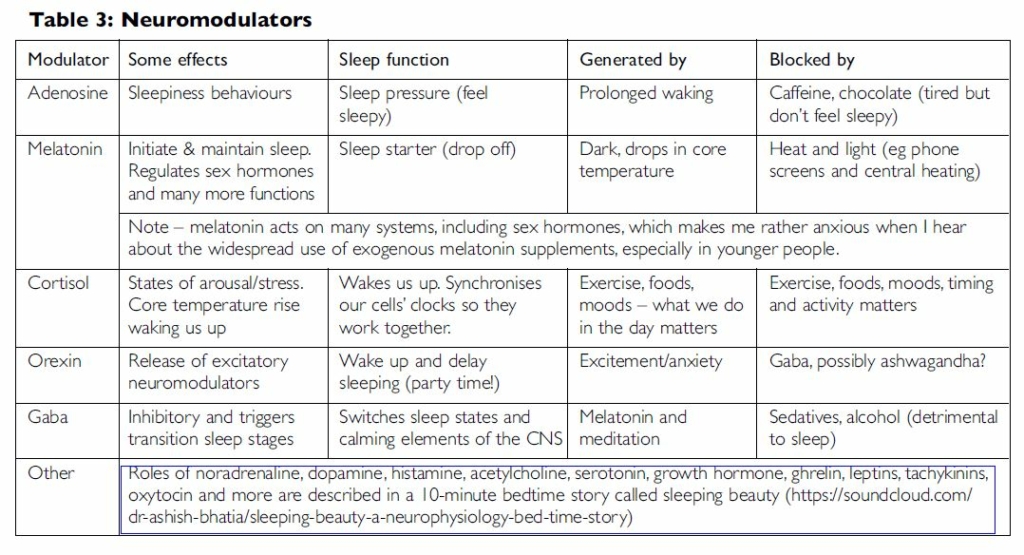
2. The nervous system (and the rest of the body) is not inactive in sleep; rather it very actively transitions between many different states. Indeed, during REM (rapid eye movement) sleep, brain activity picks up, nearing waking levels (see Tables 1 and 2 for sleep phases).
3. We enter different states of consciousness when we sleep. If we have slept poorly, microsleeps can unknowingly occur as parts of our brain trying to catch up while we are awake. This is a powerful factor in accidents, errors, and presenteeism which costs the UK economy £40 billion a year (Hope, 2016). Also, it is sobering to consider that impaired judgement and insight in a person (for example an on-call doctor) who has been awake for more than 16 hours is comparable to being well over the alcohol limit.
4. We sleep in cycles of approximately 90 minutess. So it is natural to wake at night during phases of the sleep process. This is a source of anxiety for people with insomnia who often lie awake in bed worrying about not sleeping.
A humble definition of sleep
I find it useful to think of sleep as an active, cyclical, synchronised process which occurs in all lifeforms, for internally reorganising and nourishing them by temporarily reducing contact with the outer world. Or as Shakespeare so much more eloquently put it, sleep is the ‘Chief nourisher in life’s feast’ (1606).
Many non-human phenomena are like sleep situations where things seem quiescent on the surface, but with lots going on below the surface, for example the active processes in the roots of seemingly dormant trees in winter. In my NHS sleep support groups, these similarities help highlight the subtlety of sleep processes and their connection with nature’s cycles of activity and rest. They remind us to give sleep the priority it deserves in a society that encourages us to keep going and ignore our need to sleep. This unfortunately comes at a price.
Why do we sleep?
‘Everything sleeps. If sleep doesn’t serve some vital function, it is the biggest mistake evolution ever made’
Sleep scientist Allan Rechtschaffen.
This is not an exaggeration. Every organism sleeps, and every cell of our body has its sleep cycles, during which different processes occur. These can be grouped into four categories – live, forgive, learn, and grow.
Using the analogy of a day on the beach…
Being awake is analogous to when the tide is out, and we can play on the beach. In sleep the sea covers the beach and we have to stop moving. We are no longer in waking consciousness, but because sleep returns in waves, and as the depth of consciousness changes the active processes of sleep can begin. Sleep, then is not simply unconsciousness. When we sleep we:
- Live: creatures dormant under the sand come to life and get to work. in some phases of sleep the body and mind become more active. Electrical changes, which can be detected on an electroencephalogram (EEG), show that different parts of the brain wake up.
- Forgive: Under the waves the sand gets washed through and moved around. Similarly during sleep the tissue’s cells and whole organ systems cleanse, repair and prepare for action. Our neuronal DNA repairs, immune cytokines are released and G-lymph brain cleansing processes switch on. Perhaps this is why people who consistently sleep less or badly more often develop dementia. Sleeping poorly also impacts on immunity, (infections and delaying healing), as well as our metabolism, (diabetes, obesity, cancers, strokes and heart attacks). It may also initiate inflammatory processes (implicated in auto-immune, gut, mental health and fertility issues) and disturb our emotional processing (anxiety, depression, PTSD and aggression) (Medic et al, 2017; Pace-Schott et al, 2015).
- Learn: the incoming waves pick up and move the flotsam and scattered seaweed into tidy lines high up on the shore; the sand is smoothed out ready for new footprints and sandcastles when the tide goes out. During sleep the brain’s neuroplasticity allows short term memories to integrate into long-term storage pathways. These processes enable us to be fresh and receptive to new waking experiences. Their timing and quality is important, otherwise memories get disorderly, so if we sleep poorly it will be more difficult to learn (Diekelmann & Born, 2010).
- Grow: incoming tidal currents erode the shoreline, making more sand and extending the beach. Similarly, during deep sleep hormones such as melatonin and growth hormones are released which have profound body-wide effects. They allow us to grow fitter (through changes in fat metabolism and muscle growth), stay younger (through lengthening and repair of DNA-protecting telomeres) and get smarter (by developing new neurological pathways) (Walker, 2018).
These are just a few reasons why the quality and quantity of sleep are really important. It’s also worth noting that the timing of sleep matters too. To sleep well, you need to catch the waves when the tide is right. Unfortunately, if we miss waves, then on that night we miss the opportunity to regenerate. And missed sleep is not easy to catch up on.
How do we get to sleep?
The coordinating forces of tide, wind, shore and swell generate the waves on a beach. In comparable ways sleep too is a cyclical process subject to wider influences. It will function at its best when the body (physiological processes), mind (neuro-psychological processes), environment (daily and seasonal rhythms) and social factors co-ordinate and work harmoniously.
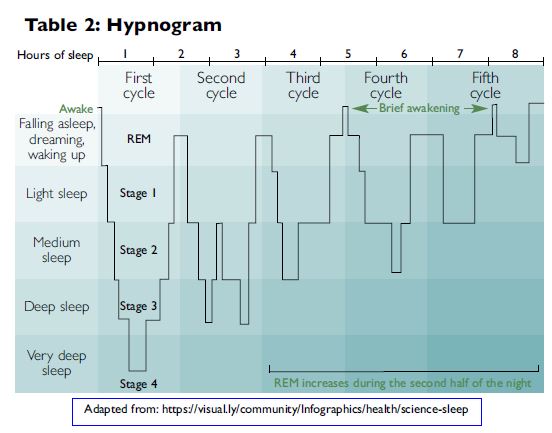
Life on our planet evolved within the daily cycle of night and day, and the annual round of the seasons. Across many species the natural starter for sleep was the sun setting. The darkness and drop in temperature would trigger the release of a melatonin (the sleep starter) and GABA (the trigger to transition into different phases of sleep). This 24-hour circadian cycle is adapted to seasonal shifts (infradian rhythms) and synchronised with our body and brain clocks (which also have ultradian rhythms of around 90 minutes). Many other neuromodulators are also involved, some of which are shown in Table 3.
Sleep waves
During a typical night we sleep in four 90 minute cycles (ultradian cycles) like waves on the beach. And within each wave we have different phases in the sleep (see Table 2). During the early part of the night we prioritise essential deep sleep, and the less urgent but still important REM (rapid eye movement/dream sleep) in the latter. These phases are modulated by some of the neurotransmitters shown in Table 3 which are sensitive to factors like light, exercise, foods, temperature, stress and drugs. So what we do in the day impacts on sleep depth and quality. Also important to note is that it is natural to be awake for short periods between these sleep waves. Indeed it is common to wake six or more times a night although we may have little recollection of doing so. Obviously, lying awake worrying about being awake as a result of this natural cycle and struggling to get back to sleep could (and often does) lead to insomnia.
So how are you sleeping?
Try the questionnaire below which contains questions about both your sleep skills and experiences.
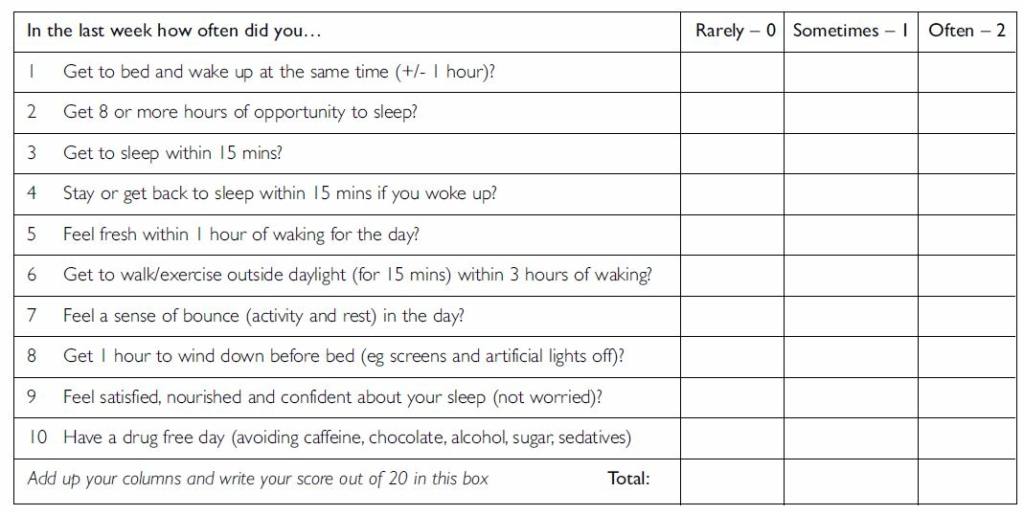
How do you feel about your score? Above 15 is good but wherever you begin will be OK because most people can improve their sleep. To begin with, just choose one easy thing to improve that you learn from this article and repeat the questionnaire after a week. It can take time to change so please be self-kind and consistent with the change you’re aiming to make.
Not sleeping well?
You are not alone. Approximately 70% of adults worldwide appear to be short sleeping, with more than 10% experiencing insomnia. It’s a common presentation in my work – around 40% of GP consultations feature people reporting difficulty getting to sleep, staying asleep, experiencing unrefreshing sleep or worrying about their sleep (Everitt et al, 2014). The good news is that many people with insomnia are probably getting more sleep than they realise and can improve their sleep with the right support.
Sleep is so fundamental to all of our health that virtually any health condition is made worse if we sleep poorly and will tend to improve if we sleep better. This
realisation led me to explore sleep, train in cognitive behavioural therapy (CBT), develop my own Humble sleep methods and to start running NHS sleep groups. This was ‘humbling’ for me because it revealed a conundrum, in that most people are short of sleep, and with detrimental consequences, but are blissfully unaware. However, when they first realise this, their satisfaction with sleep may get worse and they may even lie in bed worrying about it! Nonetheless in view of sleep’s far-reaching health benefits, raising awareness about poor sleep is important for long-term public health.
So why aren’t we sleeping?
We sleep about two hours less than our grandparents did, so what’s changed in 100 years?
Stress
- More stressors and fewer physical outlets to release distress, eg phone notifications.
- Sensationalisation in the media generates more
perceived unactionable threats..
Stimulants and sedatives
- Caffeine, chocolate, sugar, alcohol, media, lighting, prescribed drugs.
Sitting indoors
- Insufficient sunlight (especially morning) and being sedentary.
Screens
- Blue light at night (especially from phones and overhead lighting) suppresses melatoniin
Softies
- Central heating (preventing cooling at night).
- Sanitation (so we don’t urinate outside in the morning and get a dose of daylight).
Social expectations
- Social synchronisation (ignoring natural rhythms), over-scheduling and shift work.
- Stigma ‘rest when you are dead’ and supervision (phones are difficult to switch off).
Social isolation
- Reduced touch and unsatisfying social connections generating loneliness.
Translating good intentions into healthy sleep habits
In my experience, unless you have an organic sleep disorder (eg sleep apnoea) most of us can train to sleep better. Continuing with the sea analogy, like surfing the art of sleeping well is about riding the sleep waves.
- In the right place – a dark, cool, serene bed that is only for sleep and snuggles.
- At the right time – with regular wind-down, bed, wake, and walk-in-light outside times.
- In the right state – feeling relaxed and ready (sleepy, safe, physically tired and cool).
- Right now – doing what helps in the day (optimising light, exercise, food, temperature, and stress and drugs).
Realising that sleep is important and optimising these factors should help. But unfortunately information alone won’t improve our sleep, particularly in modern sleep-challenging environments. Plus some unconscious maladaptive reinforcing behaviours that start off as coping strategies will amplify insomnia: feeling anxious at bedtime about not being able to sleep; using a phone or a video in bed to unwind; drinking caffeine to stay awake in the day; even pressing the snooze button for a lie-in the morning. The good news is this can change!
CBTi
This is an evidence-based strategy for overcoming insomnia. It combines methods to optimise thoughts, feelings, behaviours, situations and sensations to unravel the factors that predispose, precipitate and perpetuate insomnia. It typically runs over 6–12 sessions with 80% sustained effectiveness.
CBTi includes the following elements:
- sleep education – understanding the mechanisms of sleep and insomnia
- sleep restriction – regulating sleep schedule and reducing awake times in bed
- stimulus control – eliminating association between bed and arousal
- sleep hygiene – modifying unhelpful lifestyle factors and daytime behaviours
- cognitive therapy – modifying inaccurate/maladaptive beliefs about sleep
- relaxation techniques – including breath strategies, progressive muscle relaxation, visualisation techniques, helpful thought processing and mindfulness.
The typical cost of private one-to-one CBTi can be up to £100 per person per session: prohibitive for most people, but there are low-cost helpful CBTi apps such as CBTi coach for highly motivated individuals. Unfortunately many people I have met were too fatigued to struggle with the app, so in response I designed a Humble approach to sleep.
Humble sleep
Humble sleep is a simple way of improving sleep that combines elements of CBTi with behaviour design strategies in online one-to-one and group consultations. Most people see some progress in one week and significant improvements in four. Follow up at four months has shown that many people sustain this improvement and 98% of attendees recommend this service, reporting sleeping better and waking refreshed. We also recorded improvements in health and mood using validated scores.
What I call the Humble Way involves four steps
- Start where you are – get to know yourself, situation, sleep blockers and supporters.
- Choose what really matters – choose a meaningful goal in life and prioritise sleep to help you achieve it.
- Do what really helps – make it easier to sleep by designing simple incremental prompts that reinforce healthy sleep habits. We often focus on optimising eight sleepers’ skills: start the day well, light right, eat for sleep, express and exercise, pause and process, end well, be ready if you wake and set up a sanctuary. These are eight evidence-based habits that are especially effective when tailored to our chronobiology (performed at specific times in the day). Find out more at www.humblesleep.com.
- Relax and shine – take time out each day to celebrate both efforts and achievements and then make refinements to factors that influence motivation and ability to change. This makes it fun to reinforce new helpful sleep habits and maintain momentum (Fogg, 2020).
Try it yourself
Although sleep may have been overlooked in the past, I hope that reading this article has revealed its value, both inspiring and enabling sleep as your humble superpower.
Resources
Chattu VK, Manzar MD, Kumary S, Burman D, Spence DW & Pandi-Perumal SR (2018) The global problem of insufficient sleep and its serious public health implications. Healthcare 7(1), 1.
Diekelmann S & Born J (2010) The memory function of sleep. Nat Rev Neurosci, 11, 114–126.
Everitt H, McDermott L, Leydon G, y Yules H, Baldwin D, Little P (2014) GPs’ management strategies for patients with insomnia: a survey and qualitative interview study. British Journal of General Practice, 64(619) e112-e119.
Fogg BJ (2020) Tiny habits: The small changes that change everything. Virgin Books.
Hope K (2016) Sleep deprivation costs UK £40bn a year. BBC news (accessed 7 July 2021).
Huberman A (2021) Master your sleep & be more alert when awake. Huberman lab podcast #2 (accessed 7 July 2021).
Medic G, Wille M & Hemels ME (2017). Short- and long-term health consequences of sleep disruption. Nature and science of sleep, 9, 151–161.
Pace-Schott EF, Germain A & Milad MR (2015). Sleep and REM sleep disturbance in the pathophysiology of PTSD: the role of extinction memory. Biology of mood & anxiety disorders, 5, 3.
Pagel JF & Parnes BL (2001) Medications for the treatment of sleep disorders: an overview. Primary care companion to the Journal of clinical psychiatry, 3(3) 118–125.
Shakespeare W (1606) Macbeth Act 2, Scene 2.
Walker M (2018) Why we sleep. Penguin Books.