Fasting – a modern take on an ancient practice
Antonia Wrigley, Holistic doctor; BHMA vice chair; founder, Real Food Campaign
Published in JHH 18.2-Frontiers of self-care
Fasting – the intentional abstinence from all or some kinds of food or drink for health or spiritual purposes – has been practised since the dawn of civilisation.
A loss of appetite in certain disease states being recognised as the body’s natural instinct to fast to aid healing. In ancient Greece Hippocrates promoted fasting for infections and other acute illness. The priests and priestesses of Asclepius, the god of medicine, used fasting to prepare acolytes for ‘approaching the deities’.
Many of the world’s religions advocate periods of fasting. In Islam it is a dawn to dusk fast during the month of Ramadan, which is seen as a period of penitence. Judaism observes an annual fast day on Yom Kippur, the Day of Atonement. And in memory of Christ’s 40-day wilderness journey – reminiscent of a Native American and modern day vision quests – many Anglicans abstain from something they like in the period leading up to Easter. Catholics traditionally refuse meat on Fridays and all food on Ash Wednesday and Good Friday.
Why fast?
‘Fasting is the greatest remedy – the physician within.’
Paracelsus (Swiss Physician 1493–1541)
Hunter gatherers often have to go for long periods without food. But unlike bears who hibernate when food is scarce, our ancestors needed to stay alert and active so they could go and hunt or gather more food. Perhaps because of evolutionary history written in DNA our bodies are adept at switching between feasting and fasting.
In more recent times until importing food became the norm, we had to eat seasonally. Unless we had plentiful stores, food sources were sparse during the ‘hungry gap’ in early spring. Once autumn fruit and winter root and grainstores had run out, we would have been glad to survive on green vegetables and flesh if we could get them. Might it be that our body expects us to fast or at the very least to have seasonal variations in the foods we eat? Having abundant calories available 24/7 is an unnatural state of affairs and today’s widening diabesity epidemic is the price we are paying. Do we need fasting ever more urgently as an antidote to our current unnatural lifestyles?
‘Through fasting … I have found a perfect health, a new state of existence, a feeling of purity and happiness, something unknown to humans.’
Upton Sinclair (Author of The Fasting Cure 1911)
Fasting has been used throughout history because it has physical, mental and emotional (and possibly spiritual) benefits even for people in good health. Experience illustrates amply the increase in energy levels, how the mind gets clearer and with it quite commonly there is growing sense of wellbeing and even euphoria. Intermittent or periodic fasting, like calorie restriction, is likely to help prevent disease and increase healthy life span (Toledo). Fasting reduces inflammation and therefore can help with conditions such as arthritis. It’s key therapeutic role could be in reversing conditions associated with insulin resistance.
Types of fasting
 A growing body of knowledge from animal and human studies suggests that along with what and how much we eat, when we eat is also of critical importance. For instance because many of our metabolic functions are linked to circadian rhythms, restricting our feeding to daylight hours, especially to the middle of the day, may be most in tune with these physiological tides. Perhaps further research will show that we should also be changing our eating patterns to harmonise with the seasons.
A growing body of knowledge from animal and human studies suggests that along with what and how much we eat, when we eat is also of critical importance. For instance because many of our metabolic functions are linked to circadian rhythms, restricting our feeding to daylight hours, especially to the middle of the day, may be most in tune with these physiological tides. Perhaps further research will show that we should also be changing our eating patterns to harmonise with the seasons.
Fasting schedules and different terminologies vary, but there are three broad categories
Time-restricted feeding (TRF)
We fast every night when we sleep, breaking our fast with breakfast. In the 1970s it was usual to eat three meals a day, with no snacks, between 8am and 6pm which is a 14-hour fast with a 10-hour eating window (14:10). Today it is more the norm to eat up to six times a day over an 18-hour eating window!
A common TRF regime is 16:8 where meals are condensed into an eight hour window and there is an absolute fast for 16 hours where no calories are consumed.
Intermittent fasting (IF)
IF, which usually refers to frequent shorter fasts, has been popularised by the 5:2 diet where there are two ‘fasting’ days a week where calorie intake is restricted to 600 calories or fewer.
Prolonged fasting
A fast of longer than two days can be consider a prolonged fast. The Buchinger Wilhelmi clinic, founded 100 years ago, has been documenting beneficial effects from its programme which consists of broths and juices, containing only 200 calories, for up to three weeks followed by a careful reintroduction to a healthy diet.
Though not necessarily recommended, in theory someone needing to lose weight could fast with the aid of supplements, until they reach their desired weight. The longest known fast was in 1971, when a 27-year-old man survived on water and supplements for 382 days and shrank from 456 to 180 pounds (Stewart & Fleming, 1973).
Key mechanisms
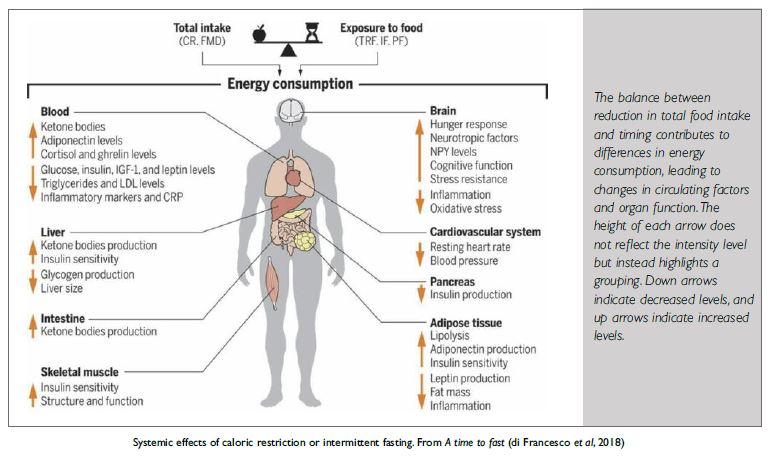
As the figure from A time to fast implies the effects of a calorie restricted diet and fasting overlap however there are also important differences which make fasting superior to calorie restriction.
Insulin sensitivity improves
Fasting is the most effective way to lower insulin levels and improve insulin sensitivity. Insulin is responsible for energy utilisation and storage. All foods raise it but carbohydrates, especially refined carbs, stimulate insulin release most strongly. This is why a low carbohydrate diet can be very effective for reversing conditions associated with insulin resistance such as type 2 diabetes. However some proteins, especially some animal proteins, notably whey, can raise insulin almost as much as carbohydrates, though interestingly (marine) collagen has been found to improve insulin sensitivity.
The body can either use glucose as a fuel source or burn fat in the form of free fatty acids and ketone bodies. When insulin levels are high, for example from a diet habitually high in carbohydrates, it is very difficult for the body to switch into fat burning mode. During a fast glycogen stores need to be used up, which may take up to 36 hours, before fully switching to burning fat. Ketosis reaches a plateau after four days of fasting by which time 75% of the brain’s energy is being supplied by ketones.
Maintenance of metabolic rate and muscle mass
Though many people manage to lose weight on a reduced calorie diet the majority put this weight back on and often even more once they resume eating normally. Also because the body quickly adapts to the continuous caloric restriction by lowering its metabolic rate, weight loss can plateau. Then the dieter may feel sluggish and demotivated. On the other hand with an intermittent or occasional longer fast our physiology continues to maintain our ability to find food. So metabolic rate is maintained, in part mediated by an increase in the hormone noradrenalin. Fasting also boosts growth hormone levels (maximal at day five) which ensure conservation of muscle mass.
Appetite regulation
How hungry we feel depends on a complex interplay of hormones, environmental cues, psychological traits and social conditioning. Fasting, if done right, can curb the appetite and subsequently lead to better appetite regulation. Ketones, produced during fasting but not on a regular calorie-restricted diet, actually reduce appetite. However, if done without knowledge and wise precautions, fasting can actually make a person more hungry.
Ghrelin, made primarily in the stomach, signals the brain that we need to eat. Production peaks four hours after a meal, but it also has its own circadian rhythm, being lowest in the morning and highest in the afternoon. When a meal is skipped, peak levels associated with mealtimes fall away again fairly rapidly and during a longer fast 24-hour production gradually falls away after the second day.
This in part explains why during a prolonged fast most people find that hunger comes in waves over the first two or three days then subsides. It’s also why skipping breakfast with time-restricted feeding feels easy and natural for many people.
Leptin is another key hormone. Leptin signals to the brain the physiological sense of fullness – satiety. Leptins are produced by adipocytes – the fat cells that primarily compose adipose tissue. In obesity, alongside insulin resistance there is a high leptin level but low satiety because of leptin resistance. When leptin levels rapidly drop during fasting it should improve leptin sensitivity and therefore appetite regulation.
Cellular ‘cleansing’ – autophagy
When the body switches to using ketones as a fuel during fasting this signals several mechanisms in the body including autophagy. Autophagy is the cellular process whereby the body recycles old and damaged parts. This is regulated by inhibition of the mTOR signalling pathway. Intermittent fasting activates the AMPK signaling pathway and inhibits mTOR activity, which in turn activates autophagy. This only begins to happen, however, once glucose stores have been depleted and insulin levels begin to drop. Intermittent fasting also reduces protein synthesis and utilisation and leads to a recycling of proteins, which is another mechanism for retaining lean body mass during a fast. As mTOR regulates cellular metabolism, growth and proliferation it has a role in cancer biology. Several mTOR inhibitor drugs have been trialled for use in cancer though currently, in part due to their side effect profile, have only a limited role.
Fasting guidelines
Contra-indications
Fasting is not recommended for children, pregnant or breastfeeding women, the frail elderly or anyone with a history of eating disorders. Caution is also advised for anyone with a low BMI and for people taking certain medications, in particular meds for diabetes and blood pressure would probably need to be reduced.
Minerals
During a prolonged water or zero-calorie fast adding minerals to water is advisable. There are many proprietary blends of sodium, magnesium and potassium for fasting and ketogenic diets. A good alternative is to consume some vegetable or bone broth or a little vegetable juice or lemon juice.
Insulin regulates salt and water in the body. This is one reason why there can be an initially dramatic loss in weight – which will benefit those with high blood pressure and fluid retention.
Preparing for a fast
Preparation is the key to success especially for a longer fast. If one’s diet includes much sugar, alcohol or caffeine then stopping them abruptly can cause withdrawal effects. It may be sensible to wean off over a week or two before a fast and eat a only real whole foods.
Breaking the fast
For a number of reasons it is important to eat the right foods on breaking the fast.
When food is reintroduced mTOR is reactivated leading to cellular and tissue regeneration. So give your body the very best available while you’re rebuilding. The saying ‘we are what we eat’ could hold true at this important time.
If it has been a longer water fast the digestive system will need a few days to get back to full functioning so at first it will only tolerate small easily digested meals.
For those fasting to lose weight it is important to know that carbohydrates can cause a rebound hypersecretion of hungry-making ghrelin. So breaking the fast on to a low or slow carb diet with adequate protein may help control your appetite.
A fast is the ultimate elimination diet. Food intolerances (usually unrecognised) can contribute to many health issues including auto-immune conditions and chronic inflammatory problems – perhaps even to everyday vague long-term but non-clinical unwellness. It might be that food restriction will reduce such symptoms. If that were to be the case then it would be sensible to use the post-fasting opportunity to continue on a relatively limited diet (with appropriate expert support) for a time before re-introducing the sorts of foods that are commonly problematic – wheat, soy, eggs and dairy – gradually while making a note of any return of symptoms.
References
de Toledo FW, Grundler F, Sirtori CR & Ruscica M (2020) Unravelling the health effects of fasting: a long road from obesity treatment to healthy life span increase and improved cognition. Annals of Medicine, 52:5, 147–161.
Di Francesco A, Di Germanio C, Bernier M & de Cabo R. A time to fast. Science 362(6416) 770–775.
Salehi A, Gunnerud U, Muhammed S, Östman E, Holst J, Björck I & Rorsman P (2012) insulinogenic effect of whey protein is partially mediated by a direct effect of amino acids and GIP on β-cells. Nutr Metab (Lond) 9, 48.
Stewart WK & Fleming LW (1973) Features of a successful therapeutic fast of 382 days’ duration. Postgraduate Medical Journal, 49, 203–209.
Zhu C, Zhang W, Mu B, Zhang F, Lai n, Zhou J, Xu A, Liu J & Li Y (2017). Effects of marine collagen peptides on glucose metabolism and insulin resistance in type 2 diabetic rats. J Food Sci Technol, 54(8) 2260–2269.
Further reading
The complete guide to fasting: heal your body through intermittent, alternate-day, and extended fasting. Jason Fung & Jimmy Moore. Victory Belt Publishing, 2018.