By Jen Unwin, Clinical Psychologist and Dr David Unwin, GP
This post has been re-written in full
We work together in a GP practice to bring psychology into the GP realm.We realised that psychological theory can seem complex and time consuming to translate into general practice. However, a large proportion of consultations are for physical and mental health conditions exacerbated by behavioural/lifestyle factors such as smoking, alcohol consumption, inactivity and poor nutrition. Doctors often lack the confidence and competence to address these issues in clinic, assuming a lack of patient motivation or fearing opening a can of worms in an all-too-short consultation.The result can be worsening wellbeing, repeat consulting and poly-pharmacy. We have devised a simple four-step plan that we have been using in 10-minute GP appointments for more than 15 years. It enhances the hope that people have for achieving their personal goals and hence their ability to make significant and lasting positive changes in their wellbeing and health. Specifically it is part of an approach that has helped us achieve drug-free remission for 57 people with type 2 diabetes, along with significant practice drug budget savings (Unwin and Unwin, 2014).
He is the best physician who is the most ingenious inspirer of hope. Samuel Taylor Coleridge
Hope is what makes us strong. It is why we are here. It is what we fight with when all else is lost. Pandora
The importance of hope
Hope has been defined as the belief that pathways exist towards our desired goals and that we have the motivation and skill to pursue those pathways. Hope is the belief in a preferred future. A positive psychology researcher, Charles Snyder (2002), summarised the research in this area. Hope is a major component of wellbeing and adjustment to adversity. High hope individuals have greater self-reported wellbeing and health. They are actually less likely to get ill and cope better if they do (Unwin et al, 2009; Billington et al, 2008). They consult less. They even live longer. Hopeful people are happier and happy people do better on a whole range of metrics related to health and wellbeing (Diener and Chan, 2011; Unwin and Dickson, 2010).
Perhaps that is not too surprising. However, what is surprising is that the powerful effects of hope on wellbeing are so rarely harnessed in healthcare settings. In fact, it is often the exact opposite. Consultations focus for the most part on what is wrong with people (symptoms) and possible risks to health. This negative emphasis can result in greater patient anxiety, unnecessary prescriptions and tests that do not lead to enhanced patient self-efficacy but instead increase learned helplessness.
Another way to understand the importance of hope is to look at research into the power of the ubiquitous placebo effect. The placebo effect is hope in action. Doctors should seek fervently to harness the power of hope in their consultations, by enhancing belief in an achievable preferred future (Frank and Frank, 1993). As a result of focusing on hopeful consultations patients become heroes rather than heartsinks, and clinicians are uplifted and sustained by hearing stories of success on a daily basis (Unwin, 2005).
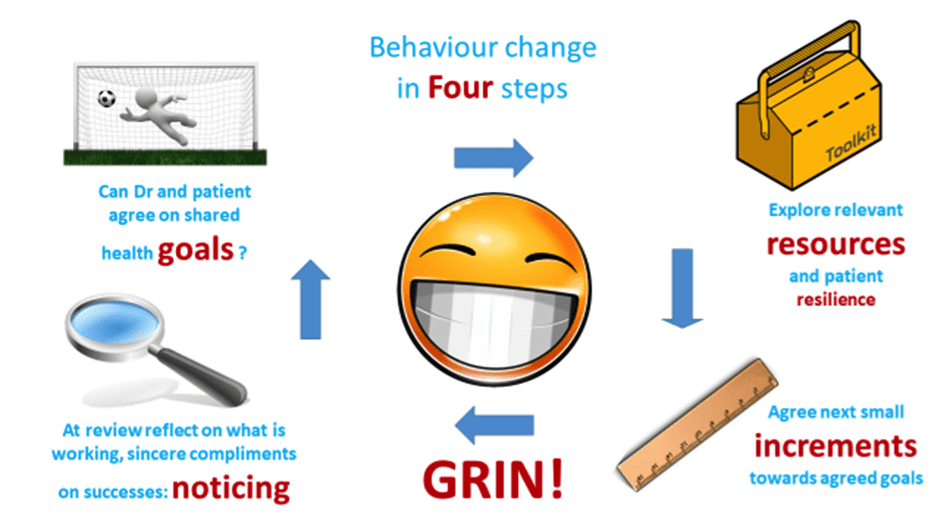
A simple model to enhance hope: GRIN (Goals, Resources, Increments, Noticing)
Our simple conversational model is based on enhancing hope by using questions from a solution-focused approach (O’Connell, 2012). Solution-focused therapy started as a form of brief family therapy in the US but is now widely used in health, education and business settings. This approach assumes that people already have the knowledge and skills to move towards their goals or ‘preferred future’ and that the helper’s role is to uncover that confidence and motivation by asking useful questions.
The approach we have developed in primary care has four stages that can be pursued in any order but always keeping in view an understanding of the person’s goals or ‘preferred future’. We have used the techniques described in direct patient work, groups and even remote digital interventions to help people with type 2 diabetes achieve significant improvements in control (Unwin and Tobin, 2015; Unwin and Unwin, 2014; Saslow et al, 2018).
Step 1 Goals
The first and most important step is establishing what ‘better’ would look like to the patient.
‘What are your best hopes for our consultation today?’
If in six months’ time, things were how you wanted them to be, what would that look like?’
‘Are there any particular ways you would like your health to improve?’
Usually people will come up with concrete goals such as ‘I want to breathe better’ or ‘I want to have no pain in my knees’
The clinician will then find a rich vein of information, motivation and insight into the person’s values by following this up.
‘What difference would that make to your life?’
Patients then respond with something of importance to them. For example, someone might say ‘then I can help with my grandchildren more’ or ‘I could keep walking the dog’.
This then allows the clinician to feed back to the patient what they have now learned. For example, ‘It sounds like family is really important to you’. A very useful question in this approach is ‘what else?’ allowing more rich information to emerge.
‘You would be able to keep walking the dog. What else?’
Step 2 Resource
The second stage is to explore what is already working in the patient’s life that is going to help them make progress. This enhances the person’s belief in their abilities to make changes. An alternative is to ask for an example from the past, e.g. ‘Have you ever managed to lose weight in the past? What seemed to work then?
Who is supporting/helping you right now?
Or might do so?’
‘What helps your now? When are things even slightly better?’
‘What has helped you in the past?’
‘What personal strengths do you have that could help?’
‘What else?’
Sometimes the strengths question is difficult for people to answer. A different slant can be to give the person a sincere compliment based on what you already know of them, or to ask what a loved one would say.
‘I know you are a very determined/organised/ positive/caring person and that this will help you to make good progress.’
‘What would your wife/best friend say are your best qualities?’
‘What else?’
Step 3 Increments
So many people have goals they never realise because they fail to take those first small steps towards their goal. So the third stage of the conversation is either about what would be happening if the person first started to make progress and what they might notice when they do, or committing to some specific ‘small steps’ they think would be helpful.
‘What will be the next small sign that you are making progress?’
‘What will your wife/best friend notice that will tell them you are making progress?’
‘What will tell us you are making progress?’
‘Bearing in mind your goal, can you think of a small change you can easily make before we meet again? ‘
‘What else?
This last question can lead to permission for regular measurements and tests such as waist circumference, weight, BP or HbA1c, for example.
Step 4 Noticing
So often the medical paradigm is about noticing negative things like pain or depression and asking how bad it is. In this model we are trying to shift the focus to positive experiences by asking what is working and what a person has noticed about any improvement. These questions are very useful at follow-up appointments to keep the conversation ‘progress focused’.
What is better since we last met?’
‘What difference has that made to you?
Who else in the family noticed?’
‘What seems to be working well for you right now?’
‘What else?’
The healthcare professional should also be attuned to noticing progress and giving positive feedback.
‘I have noticed that you are smiling more/came without your stick/are breathing better this week.’
‘Your tells me that you have been successful in making important changes…’
‘Wow! You have lost 3″ off your waist. How did you do that?’ (get details)
We have found that patients respond really positively to graphs of progress printed from the EMIS GP computer system (see example below) and like to show family and friends how much progress they have made. In a nutshell noticing supplies feedback
Wider application of the model
The process of shared goal setting, acknowledging what is already working, identifying the next steps and noticing progress is a simple model that can also be applied to meetings, supervision, appraisal, family and personal goals.
What are our best hopes for this meeting today?’
‘Where do I/we hope to be this time next year?’
‘What is already going well in our team?’
‘What strengths do we have in the team?’
‘What will tell me I am managing you better?’
‘When have I noticed myself being at my best recently and how did I do that? ‘
‘What have I/we been pleased to notice in the last week?’
‘What else?’
Using a solution-focused approach challenges the traditional model that any problem must be understood and analysed in detail before progress can be made. It gets away from ‘diagnosing’ the problem to envisioning the solution. Most clinicians believe that taking a history detailing the causal events that led up to illness is always important in finding the remedy. In fact, though this may help understanding, sometimes it can hamper progress. For example, patients may have experienced extremely difficult childhoods but examining the details of just how traumatic can sometimes lead to people feeling worse. In a case like this, particularly if time is short, an alternative could be to notice resilience with a sincere enquiry about ‘toughness’ by asking, ‘that sounds so hard, I’m interested to understand how you managed to get through those difficult times?’ This may be an excellent prelude to exploring goals, and a much more productive and cheerful use of time than taking your patient through a very painful, detailed examination of half-buried trauma. In this way progress can be fast and sometimes surprisingly so. Practitioners must be ready to give up ‘advice’ and have faith in the patient’s expertise and strengths. The practitioner’s knowledge and experience is then used to support the patient’s efforts and progress. We have found this approach to be easily incorporated into a wide range of clinical scenarios. It is positive, patient-centred and less burdensome on staff. Surely, this is much needed in helping both patients and staff remain happy, resilient and well.
A GRIN case study and full references can be found in the downloadable version of this article.