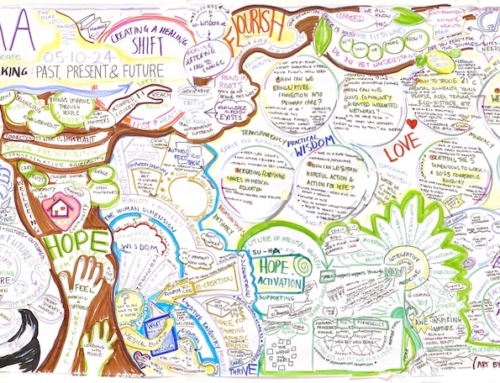
What is holistic healthcare?
An interview with Dr Marina Malthouse
We’re not made up of body parts. We are whole.
Interview script
Marina: My name is Marina Malthouse and I’ve worked as a doctor for 33 years and I was in palliative care for 20 years. People who were dying, required me more as a human being, than as the classic ‘Orthodox approach to medicine’-type doctor. What I do is combine nature and an approach to life, which means being passionate about food ,and growth, and bodies, and people, and relationships ,and connections… and some academic work as well.
Ashish: What does holism or holistic care mean to you?
Marina: It means a lot! I think there’s a holistic care to life, which I very much think I found. It was an important factor in my mother’s life.
My mother was Greek and she was also a doctor. My upbringing was very holistic, actually, in our family. Her way of thinking, was a way of considering the health of the body and the mind. Was all one. So to me, it felt quite different going to medical school, where we were focusing very much on these disease entities and all this sort of stuff, this knowledge. Somehow, my mother, when I used to talk to her about that, she had already managed to wrap all that into one.
Whereas I found it difficult because I’d been raised in this very holistic way. But now I was seeing the person, as the patient, as the body. It was very disparate from what I felt growing up. So, the holistic approach felt very natural to me. And in the end, I feel that was how I ended up practicing in the world of palliative care. If I couldn’t come to the patient as a whole person myself, as the doctor, and see and interpret and be with the person who was going to die, inevitably, in palliative care, then I didn’t think I could be a good doctor to them.
Ashish: What does holism mean?
Marina: It means whole! I had such a strong perception of that growing up. Because to my mother holism was so important – mind, body, and soul – it felt natural to me. But like I say, I did have to work at it because medical school had a very, very convincing way of training us, I think. And the environment that we worked in, there wasn’t the psychology of talking about “how do you feel?” We’re not made up of body parts. We are whole, and I have a very strong sense of that.
I became a patient quite early on in my young medical life. And that helped me see patient experiences subjectively, and assess objectively how I had been trained. I was then on the receiving end as a patient at the age of 24 with a lymphoma, and being treated by other doctors, totally with regards to my physical body. But I knew I felt so much more than just the disease that was being treated and managed.
So I had that to help me develop, I hope, into a doctor and a person who really focused on seeing the person as a whole.
Ashish: What are the challenges to practicing holistically?
Marina: Oh, I think number one is time. I think ,we in the medical profession, have been robbed of time. As you can imagine many, many people who had a terminal illness, had often looked into alternative practice, complimentary medicine. They would be praising them, as opposed to the doctors, that they had been treated by. And I always used to think, “well, yeah, you’ve got an hour with an alternative practitioner, if doctors had an hour with you, you’d think they were a lot nicer!” Because they [the patient] had often had quite difficult experiences in the busy medical environments of oncology outpatients and on and off the table having radiotherapy or whatever it was. So I think time is a huge, challenge to practice holistically.
And I also think the environment, that we work in. Which are not terribly, um, warm and cozy. That is definitely what we had and the hospice, I would say they are much nicer spaces to see people. I would often have a consultation sitting outside on a bench, in the garden of the beautiful grounds of the hospice. So we had a very holistic environment – listening to the birds, feeling the sun on our skin, whilst chatting and engaging.
Ashish: What excites you about the opportunities in the future?
Marina: What excites me, is seeing far more in the literature, particularly talks and different websites that are concerned with this kind of approach.
There’s much more acceptance and integration of alternative and complimentary medicines, and the approach of functional medicine, integrated medicine. The creative arts that are now becoming more commonplace – even down the hospital corridor. Or the fact that hospital managers now know that what you have outside in the garden, as you walk along the hospital corridor, actually matters! So rather than face brick walls, interesting spaces have been developed.
And we’re actually talking now about wellbeing of doctors. Thank you to COVID actually. Everybody knows doctors have a high stress response based on what they’re practicing every day, and suffering all the more for it with high, higher suicide rates. But now there’s so much talk about the wellbeing of doctors, and others in health care. Because happy doctors and happy healthcare staff will care for patients better…FACT!
So, that’s what I’m encouraged by. We’re paying attention to something that has long been lacking.
Ashish: What would you say to a healthcare student just starting out?
Marina: I would try to get them to really see that the patient, the person they have in front of them, is somebody that matters. They’re not so-and-so in bed, such-and-such with breast cancer. However busy they are, they need to just to make that person feel cared for. That person who is vulnerable in the hospital bed. We’re all vulnerable when we are ill. Make them feel like they matter. A smile doesn’t take long. Just to touch of a hand if it’s appropriate. Just exchanging some form of very meaningful contact. That’s going to make that person feel that there’s somebody there who reminds “me that I am this person”. So that is a very important thing to me because I’ve been on the other side a few times and it’s something I always felt needed to be relayed.